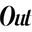While you’re in that awkward middle period where you’re old enough that you can strain your back while you’re sleeping and clubs are getting “too loud,” but not old enough to hit that hot Older Wiser Lesbian (OWL) phase yet, perimenopause is going to come knocking at your door.
Most of us have at least a vague idea of what to expect when our periods take a permanent hiatus, but many people are clueless about perimenopausal symptoms and what can be done about them.
Which is a shame because these symptoms can greatly affect your mood and sex life, and there steps you can take to address them. To this end, medical experts share advice ahead.
What is perimenopause?

Two lesbians
Cultura Creative/Shutterstock
Perimenopause is the transitional phase before your periods stop altogether — also known as menopause — when your estrogen and progesterone levels begin to fluctuate and decline in unpredictable ways. Perimenopause usually starts when you are in your 40s, but symptoms can begin earlier.
“Changes in your period are often the most-noted symptom,” said Dr. Kathleen Jordan, the chief medical officer for Midi Health. “Your cycles might initially get shorter and more frequent, intermittently heavier, and then later in perimenopause become more spaced apart. You can also intermittently experience menopausal symptoms like hot flashes, ‘brain fog,’ worsening anxiety or depression, night sweats, or trouble sleeping.”
Perimenopause symptoms can develop slowly over the course of years and can start off with small changes that you might not notice right away, according to Shaira Daya, a registered dietitian and perimenopause nutritionist.
“Some of the early symptoms of perimenopause can be as simple as your period just feeling different,” she said. “Your period may be more frequent or shorter in length. Bleeding may be heavier, lighter, or accompanied by bloating, cramping, or headaches that you never used to experience.”
What treatments are available for perimenopausal symptoms?
Estrogen.
BLACKDAY/Shutterstock
A lot of women ignore the symptoms that come along with perimenopause because they’re not always as extreme as they become with menopause. Many are also not taught about this transitional period, but there are treatments available.
The estrogen and progesterone therapies that are a part of Menopausal Hormone Therapy (MHT) can also be used to treat perimenopause. “One does not need to wait until full menopause to experience the symptoms, nor do they need to wait until full menopause to benefit from hormone therapy,” Jordan said. “Often women start these hormone therapies in perimenopause and they benefit from them all the way into menopause.”
Doctors can also prescribe low-dose birth control to treat hormonal fluctuations since this treatment contains estrogen and progesterone. Then, once you hit menopause, you can be transitioned off of the birth control pills and onto MHT.
But if you don’t want to start taking hormones, there are other treatments that can also offer symptom relief.
“For patients who prefer not to use hormone therapies at all or can’t use them, there is still plenty to do to feel better and do better in perimenopause,” she said. “There are non-hormonal medications that can help with symptoms — these approaches vary based on the symptom. Other lifestyle changes, like implementing more strength training and adjusting sleep hygiene and/or adjusting your diet help too. Sometimes these adjustments are done with medications and sometimes doing these things without medications helps, too.”
Daya said that changes in nutrition can help all on their own or work as an accompaniment to hormonal treatments: “Rebalancing the diet to meet your stage of life is a necessary step towards feeling good in your body through midlife, and reducing your risk of age-related health conditions like cardiovascular disease.”
She recommended a diet rich in fruits, vegetables, fermented foods (for gut health), as well as oily fish like salmon, mackerel, and sardines, which “contain high amounts of omega-3 fats that reduce inflammation and maintain, lubricate, and improve elasticity of mucosal tissue – including the cervix."
Should you talk to your doctor?

Doctor holding a stethoscope.
PeopleImages/Shutterstock
Since there isn’t a way to know exactly when perimenopause starts, and not all doctors are well-educated on the topic, it can feel overwhelming to know how to talk to your doctor if you think you are experiencing perimenopausal symptoms.
“Unfortunately, most clinicians haven’t been trained in perimenopause and don’t often consider how many seemingly unrelated physiological symptoms might be due to perimenopause,” Daya said. “Find a peri- or menopause-specific provider to help you understand what’s happening and what treatment options may be available to you that align best with your lifestyle.”
And don’t be afraid to ask your primary care doctor or OB-GYN to refer you to a menopause specialist — because you have a right to see a doctor who can help you make informed decisions about your health. “Every woman deserves an informed conversation on these changes. Not all OB-GYNs are trained in menopause and perimenopause, so ask for one that is,” Jordan said.
What should transgender men know about perimenopause?

Trans man holding a trans Pride flag.
Oscar M Sanchez/Shutterstock
Transgender men who have ovaries and a uterus are likely to experience many of the same symptoms that cis women do, including mood changes, hot flashes, and changes in sex drive, but the emotional toll it can take can be more intense, especially for those already experiencing gender dysphoria, said Sofie Roos, a bisexual licensed sexologist, relationship therapist, and author at relationship magazine Passionerad.
Finding a trans-inclusive doctor who understands your unique challenges will be the key to getting effective treatment as you go through perimenopause.
“I meet queer men everyday in my work, and for the ones afraid of seeking help from a doctor, I recommend to bring a friend or a partner as support, to write down your symptoms beforehand and bring them with you, to find a trans-inclusive health care provider — which you can find by taking help of the LGBTQ+ community where you live — and to always remember what you have the right to respectful health care that makes you feel seen, understood and that helps,” Roos said.
Daya said you also shouldn’t be afraid to stop seeing a doctor and look for someone new if you aren’t being listened to or you don’t feel comfortable with them. “It’s so important to find a provider you’re comfortable talking to about all your concerns – including sexual health – and who will take what you have to say seriously,” she said. “If you feel that you’re not being listened to or that your concerns are being dismissed, please find another provider.”
Will perimenopause impact your sex life?

Two women lying in bed, one with her head in the other's lap.
Zamrznuti tonovi/Shutterstock
As your hormones begin to change during perimenopause, you may notice a drop in libido, have trouble getting aroused or reaching orgasm, and experience vaginal dryness. This can be especially tricky in lesbian or sapphic relationships when both partners are going through this change at the same time.
"You may find that your body takes longer to become aroused or that certain toys or positions feel different than they used to,” Jordan said. "These changes are real. We have changes in our sensory receptors and the skin of the vulva and vagina can become thinner and less elastic, making things feel differently.”
But beyond physical changes to your body, perimenopause can also cause emotional and mental changes that can impact your sex drive. “Symptoms like the fatigue associated with insomnia, rising stress, and/or relationship issues can also impact libido, so it’s important to look at the holistic picture of all that is going on in midlife to support your best sexual health,” she explained.
Roos said that queer women often have far less information about sex during perimenopause than their heterosexual counterparts, which can make you feel even more confused or alone, but luckily there is one side benefit to being in a lesbian or sapphic relationship.
“In queer sexual relationships where both have a vulva, the perimenopause is generally easier, as vulva to vulva sex isn’t as focused on penetration, which makes it easier to adapt the sex life to what feels good right now,” she explained.
What can you do to improve your sex life during perimenopause?

Two sets of women's hands grasping in bed.
Iryna Kalamurza/Shutterstock
To deal with sexual dysfunction, changes in libido, or vaginal dryness that come with perimenopause, Jordan recommends investing in a high-quality water-based silicone lubricant, asking your doctor about prescription vaginal estrogen cream, which is “a local, non-systemic treatment that restores the health of the tissue without affecting your whole body,” and working on your pelvic health.
“I'd also say that perimenopause is also an excellent time to expand your definition of intimacy,” Jordan said. “Focus on sensory play, external stimulation, and open communication with your partner about what feels good in the moment.”
Communication will be key during this time if you want to keep having good sex because “the lust and your preferences and boundaries tend to change,” Roos said.
“Explore more than the ‘usual,’” she recommends. “Sex doesn't need to look a certain way, so explore new ways to touch, give oral, use sex toys and don’t be afraid to lower the tempo, and then be playful and communicate around what feels good, and I’m sure you’ll find new pleasurable ways of stimulating each other.”